The Wisconsin Perspective: How Artificial Intelligence Could Shape Regional Anesthesia Education and Ultrasound Training
Cite as: Resop A, Schroeder K. The Wisconsin perspective: how artificial intelligence could shape regional anesthesia education and ultrasound training. ASRA Pain Medicine News 2025;50. https://doi.org/10.52211/asra080125.005.
Artificial intelligence (AI), a field of computer science that focuses on creating algorithms that imitate human decision-making, is being integrated into various aspects of clinical and educational systems in anesthesiology. AI algorithms have not yet surpassed human performance in all domains, but their ability to quickly and accurately sift through large volumes of data and uncover correlations and patterns could be valuable for teachers and clinicians. While the procedure-based nature of anesthesiology offers several protections from AI encroachment, we must begin to embrace what AI has to offer in the development of the education curriculum.1
To effectively understand the current state of AI, a working knowledge of commonly used terminology is helpful. “Deep learning” uses artificial neural networks to model activities that would normally be accomplished by a human brain, and large language models (LLMs) use “deep learning” paired with large data sets to “comprehend, generate, and predict new content.”2,3 LLMs have recently gained widespread interest due to their incorporation into popular operating system platforms. For example, the use of AI platforms has now been democratized and made available to everyone, no longer the exclusive domain of those with the time, resources, and background or connections to train their own AI platform. Literature searches describing the use of AI in anesthesiology demonstrate how it can be utilized to target depth of anesthesia monitoring, predict adverse events, risk-stratify patients presenting for surgical procedures, predict clinical outcomes and post-operative complications, assist in the management of acute and chronic pain conditions, and improve operating room logistics.3 Less commonly described in the literature is the use of LLMs in the creation of education curriculum, but interest in this application is beginning to emerge.
Education remains a pillar of academic institutions where there is an expectation to provide comprehensive and targeted anesthesia training to a diverse set of learners, ranging from medical students and clinical anesthetists to resident and fellow physicians. It is not uncommon for regional anesthesia education to also need to be translated into different subspecialties with varying backgrounds, including but not limited to emergency medicine, trauma surgery, critical care, and physical medicine and rehabilitation. There are also opportunities to provide ongoing medical education training to colleagues who may have trained in an era before the widespread utilization of ultrasound imaging or the incorporation of novel fascial plane regional anesthesia techniques. In addition, the accelerated pace of medical knowledge accumulation and the rapid expansion of publication numbers can be daunting for both learners and teachers in terms of staying up to date on the current literature relevant to pain management.4
Simply put, given the expansion in learner diversity and volume, clinical knowledge accumulation, and ever-present clinical demands, there is a need within the field to generate educational content both accurately and efficiently that can be easily customized. For example, an individualized curriculum can be generated for medical students rotating with the acute pain service, where the breadth of regional anesthesia knowledge is different than what would be expected for a fellow in a regional anesthesia and acute pain medicine fellowship.5 LLMs can generate learning objectives, keywords, educational content, problem-based learning discussions, and evaluation questions tailored to an individual learner and identify areas of weakness that can then be used to tailor ongoing education efforts. Using AI to create iteratively more challenging knowledge assessments may ultimately be beneficial in encouraging residents to leverage their existing knowledge and expand their understanding. Beyond knowledge assessments, AI can be used to build assessment rubrics for procedural skills and collate various components of skill performance to provide helpful feedback for residents' improvement.
Recently, AI has been implemented as a guide that aids in the identification of sono-anatomy and vital structures relevant to ultrasound-guided peripheral nerve blocks. Similar to radiologists utilizing AI image recognition for diagnostic purposes, anesthesiologists can now incorporate similar technologies into real-time ultrasound scanning procedures. AI software can annotate ultrasound imaging and may augment regional anesthesia and acute pain management education while improving patient safety. In a study Bowness et al., AI image interpretation was evaluated, demonstrating that highlighting important sono-anatomy reduced the perceived risk of unintended needle trauma to nerves, arteries, pleura, and peritoneum in 62.9% of scans, and the anticipated risk of block failure was reduced in 81.3% of scans.6
At academic institutions, attending anesthesiologists are tasked with providing excellent patient care while simultaneously educating residents. However, staffing paradigms may result in residents missing out on important baseline anatomical knowledge and understanding. In these cases, a resident physician may be guided to correctly and safely administer local anesthetic under the direction of an attending physician without fully understanding the ultrasound image and pertinent sonographic anatomy that allows for the safe performance of a particular regional anesthesia technique. In this setting, AI technology can be utilized to enhance the performance of ultrasound scanning while also aiding learners in accurately identifying key structures surrounding the target nerve or fascial plane.7 This technology would also benefit inexperienced clinicians, specifically those who finished training before the adoption of ultrasound guidance for regional anesthesia procedures. According to Gugnor et al., the accuracy of labeling overlays using AI on ultrasound images for eight block regions was found to be “reliable and consistent.” However, advancing age or obesity in patients may affect ultrasound images, resulting in less consistent recognition of important structures. An additional limitation to consider is anatomic variations, for example, the branching of tibial and peroneal nerves from the sciatic nerve may be at different levels.7 There is also a concern that trainees, or even experienced anesthesiologists, may become overly reliant on imaging overlays. In these settings, it may be challenging to identify and correct inaccuracies in the overlays. Furthermore, if providers are reliant on AI overlays, they may be unable to provide safe and reliable regional interventions in settings where these smart ultrasounds are unavailable.
Recently, AI has been implemented as a guide that aids in the identification of sono-anatomy and vital structures relevant to ultrasound-guided peripheral nerve blocks.
There remain significant limitations associated with AI in regional education that deserve thoughtful consideration. Primary among these concerns are issues related to data security and privacy. Any data entered into an LLM must be de-identified to ensure that protected health information is not compromised. Additionally, it is crucial to acknowledge that AI models are typically trained on existing data, which may perpetuate biases or errors. AI-generated content also has the potential for significant errors or hallucinations; therefore, any clinical advice needs to be carefully vetted by trained physicians.8 While there has been a rise in the number and quality of AI studies in anesthesiology, it is not yet entirely clear where these models are best implemented, and further work is required. Future research should focus on developing a curriculum in a manner that best serves learners, including specific prompt language that leads to improvements in LLM education curriculum outcomes.
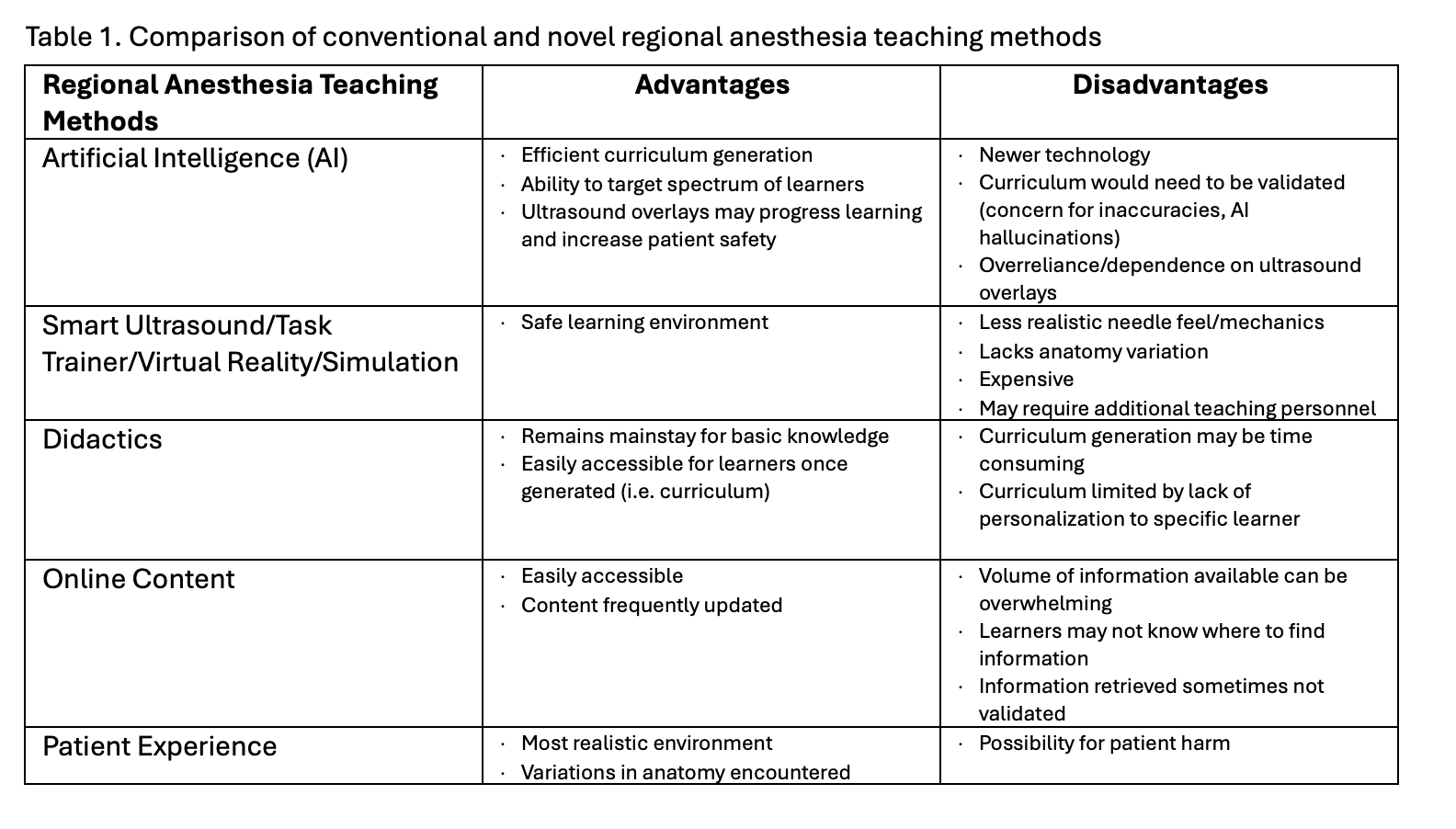
Mainstays for regional anesthesia education historically involve didactics, simulation, and, of course, applying regional interventions on real patients. Didactics will continue to be important for attaining basic knowledge. However, didactics have limitations when it comes to personalizing a curriculum for a specific learner. There have been other technologies developed involving simulation, virtual reality, and needle trainers that are promising and allow learners to practice in a safe learning environment without posing harm to real patients. However, these technologies are sometimes cost-prohibitive and often lack realistic needle feel or feedback that we observe when performing procedures on real patients (Table 1). While we will continue to implement these current teaching methods, there will be ongoing pressure to incorporate AI into diverse aspects of education and clinical care. It will be crucial for anesthesiologists to determine the best indications for this technology, establish boundaries to ensure safe and ethical application, and ensure that AI maintains its position as a tool used to augment physician expertise, not replace it.3


References
- Schroeder KM, Elkassabany N. Artificial intelligence and regional anesthesiology education curriculum development: navigating the digital noise. Reg Anesth Pain Med 2024:rapm-2024-105522. https://doi.org/10.1136/rapm-2024-105522
- Khan AA, Yunus R, Sohail M, et al. Artificial Intelligence for anesthesiology board-style examination questions: role of large language models. J Cardiothorac Vasc Anesth2024;38(5):1251-9. https://doi.org/10.1053/j.jvca.2024.01.032
- Bellini V, Russo M, Lanza R, et al. Artificial intelligence and "the art of kintsugi" in anesthesiology: ten influential papers for clinical users. Minerva Anestesiol 2023;89(9):804-11. https://doi.org/10.23736/S0375-9393.23.17279-8
- Nanda M, Grant SA. Leveraging artificial intelligence for regional anesthesiology curriculum development. Reg Anesth Pain Med 2024: rapm-2024-105906. https://doi.org/10.1136/rapm-2024-105906
- Hurley NC, Schroeder KM, Hess AS. Would doctors dream of electric blood bankers? large language model-based artificial intelligence performs well in many aspects of transfusion medicine. Transfusion 2023;63(10):1833-40. https://doi.org/10.1111/trf.17526
- Bowness JS, Burckett-St Laurent D, Hernandez N, et al. Assistive artificial intelligence for ultrasound image interpretation in regional anaesthesia: an external validation study. Br J Anaesth 2023;130(2):217-25. https://doi.org/10.1016/j.bja.2022.06.031
- Gungor I, Gunaydin B, Buyukgebiz Yeşil BM, et al. Evaluation of the effectiveness of artificial intelligence for ultrasound-guided peripheral nerve and plane blocks in recognizing anatomical structures. Ann Anat 2023;250:152143. https://doi.org/10.1016/j.aanat.2023.152143
- Grigio TR, Timmerman H, Wolff AP. ChatGPT in anaesthesia research: risk of fabrication in literature searches. Br J Anaesth 2023;131(1):e29-30. https://doi.org/10.1016/j.bja.2023.04.009