How I Do It: Lumbar Plexus Block
Cite as: Lim M, Deeble C, Sondekoppam R. How I do it: Lumbar plexus block. ASRA Pain Medicine News 2025;50. https://doi.org/10.52211/asra080125.006.
How I Do It
Introduction
The lumbar plexus block (LPB) is an advanced regional anesthesia technique in which local anesthetic is deposited within the psoas major muscle, near the lumbar plexus, to achieve blockade of the L1–L4 ventral primary rami of the lumbar spinal nerves. It is commonly employed for anesthesia and or analgesia of the ipsilateral lower limb.1,2 Often, LPB is used to block innervation to the hip, femur, and anterior and medial thigh with the advantages of preserving intact contralateral limb sensation and a lesser degree of sympathectomy with better hemodynamic stability.3
The block was first described by Winnie and colleagues in 1973 as an inguinal paravascular technique while acknowledging the possibility and advantages of a posterior paravertebral approach.4 While a conduit exists where catheters can be advanced proximally towards the lumbar plexus via the inguinal paravascular technique along the path of the femoral nerve,5 the original description of injecting local anesthetic into the femoral nerve “sheath” with an intended proximal spread of injectate and a “3-in-1 block,” where injectate spreads to the three main terminal nerves of the lumbar plexus for lower extremity blockade: the femoral nerve, obturator nerve and lateral femoral cutaneous nerve (LFCN). The obturator nerve and LFCN coverage were later contested as the inguinal paravascular injections seem to mainly block the femoral nerve and only at times, the LFCN at the inguinal area.6,7
Approaches to performing the LPB have evolved over time based on cadaver and imaging studies and technological advances in regional anesthesia.8 Advancements in nerve stimulation and ultrasound-guidance further refined LPB techniques while delineating better injectate spread.8,9 In the pre-ultrasound era, a posterior anatomical approach entailed inserting the block needle at the lateral 1/3 and medial 2/3 of an imaginary line joining the posterior superior iliac spine and L4 vertebrae and advancing the needle to contact the transverse process and deliberately walked off of it in a cephalad direction into the psoas major muscle to elicit nerve stimulation with resultant quadriceps twitching.6 Other techniques described include the “psoas compartment block” based on loss of resistance into the psoas muscle,10 and the ultrasound-guided approaches, including the “Shamrock Method,”11 a paramedian transverse scan through the lumbar intertransverse space,12 and a scan through the acoustic window of the lumbar ultrasound trident.13 Here we describe our transversal approach to the LPB using ultrasound visualization of the shamrock sign, along with neurostimulation, and pressure monitoring to maximize block efficacy while minimizing complications.
Anatomical Considerations
The lumbar plexus, the plexus of nerves formed by the anterior rami of the first four lumbar spinal nerves (L1–L4) and subcostal nerve, plays a crucial role in innervating the skin and musculature of the lower abdominal wall, pelvis, and lower extremity. The plexus lies deep within the psoas major muscle, and its branches emerge from the psoas major muscle to course toward their respective targets and include iliohypogastric (L1), ilioinguinal (L1), genitofemoral (L1-L2), femoral (L2-L4), lateral femoral cutaneous (L2-L3), and obturator nerves (L2-L4). Regardless of the technique used, it is vital to note the location of the inferior pole of the kidney and lumbar vasculature when performing the block to minimize the risk of kidney injury, bleeding, and hematoma formation.14 It is also important to consider the position of the neural foramina relative to the needle trajectory to reduce the risk of epidural spread.2
Sono-anatomically, the LPB target lies at the junction of the posterior one-third and anterior two-thirds of the psoas muscle, anterior to the transverse process of the lumbar vertebrae.15 Although the horizontal distance between the lumbar plexus and the L4 transverse process appears consistent between sexes, significant gender-related differences exist in the depth of the lumbar plexus from the skin surface. In addition, imaging studies have demonstrated a positive correlation between lumbar plexus depth and body mass index (BMI), indicating increased depth in individuals with higher BMI.10
Careful attention must be paid to the vascular anatomy in relation to the lumbar plexus to minimize the risk of bleeding complications during block placement. The lumbar plexus lies in the vicinity of lumbar arteries, which originate from the aorta on the posterior aspect of the upper four lumbar vertebral bodies and course postero-laterally, passing beneath the sympathetic trunks to traverse the intertransverse spaces of the lumbar spine before entering the musculature of the abdominal wall. These vessels are known to form collaterals with the lower posterior intercostal, subcostal, iliolumbar, deep circumflex iliac, and inferior epigastric arteries.16 While a consistent anatomical trajectory of arteries are noted in studies, variability in vascular anatomy primarily stem from the number of arterial branches originating from the aorta (ranging from two to four) and the significant variability of the lumbar venous anatomy.17,18
Given this potential for anatomical variation, especially when vascular anomalies are suspected, preoperative review of diagnostic imaging (MRI, CT images where available) and intraprocedural ultrasound scanning of vascular anatomy in the needle path is warranted to minimize the risk of iatrogenic vascular injury. Visualizing vascular anatomy can be challenging at times, as seen in a case series of octogenarians undergoing ultrasound-guided imaging, where the lateral position of the lumbar artery was visualized in only 26% of patients.19 Additionally, although the lumbar plexus nerves can be identified in more than 50% of cases with ultrasound, real-time visualization of the needle can be difficult.19 Therefore, to accurately place the needle in the vicinity of the lumbar plexus while avoiding vascular puncture, the use of concurrent neurostimulation, the use of a vascular marker in the injectate, and the practice of repeated aspiration while the needle is advanced is recommended.
The lumbar plexus block, when performed with triple monitoring to minimize the risks of neurologic and vasculature complications, provides safe and effective lower extremity analgesia.
Positioning and Preparation
Prior to initiating the block, standard ASA monitors are applied, and the patient is placed in the lateral decubitus position with the hip and knees flexed, and the side of the block is facing upward (Figure 1). Intravenous premedication, such as midazolam (1-2 mg) and fentanyl (25-100 mcg), is recommended as needed for patient comfort during the placement of this deep block. The patient is sterilely prepped from the mid-clavicular line to the midline of the spine, roughly covering a wider area at the levels of L3-L5. Important surface landmarks to note include the iliac crest, posterior superior iliac spine, lower border of the rib cage, and L3-5 spinous processes.
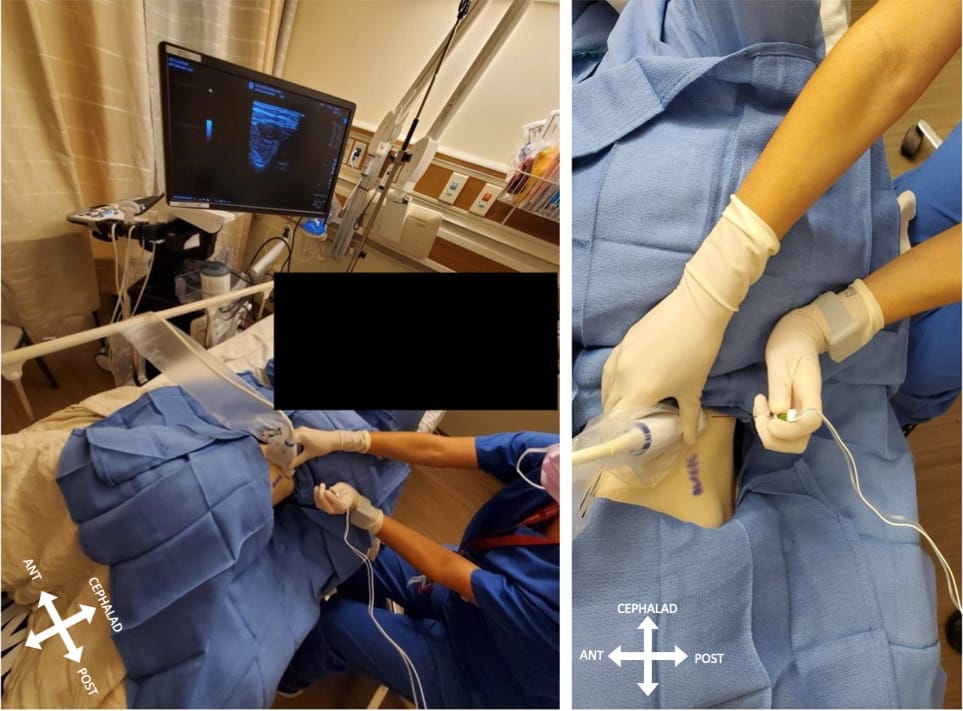
Sonoanatomy and Approach
A low-frequency curvilinear ultrasound probe is prepped sterilely into the field and placed in a transverse orientation cephalad to the iliac crest in the mid-axillary line. A low-frequency curvilinear probe allows for a wider field of view and deeper tissue penetration for this deep block. The ultrasound is used to visualize the muscle layers of the abdominal wall, including the external oblique, internal oblique, and transversus abdominis. The abdominal wall muscles are followed dorsally until the quadratus lumborum (QL) comes into view, and the QL is then followed until it inserts onto the L4 transverse process.
At this point, we aim to optimize a view of the “shamrock sign.” The leaves of the shamrock include the psoas muscle (anteriorly), QL (laterally), and erector spinae muscles (posteriorly), with the transverse process resembling the stem of the shamrock (Figure 2).11 Color Doppler is used to identify the lumbar arteries and plan for a safe needle trajectory (Figure 3).
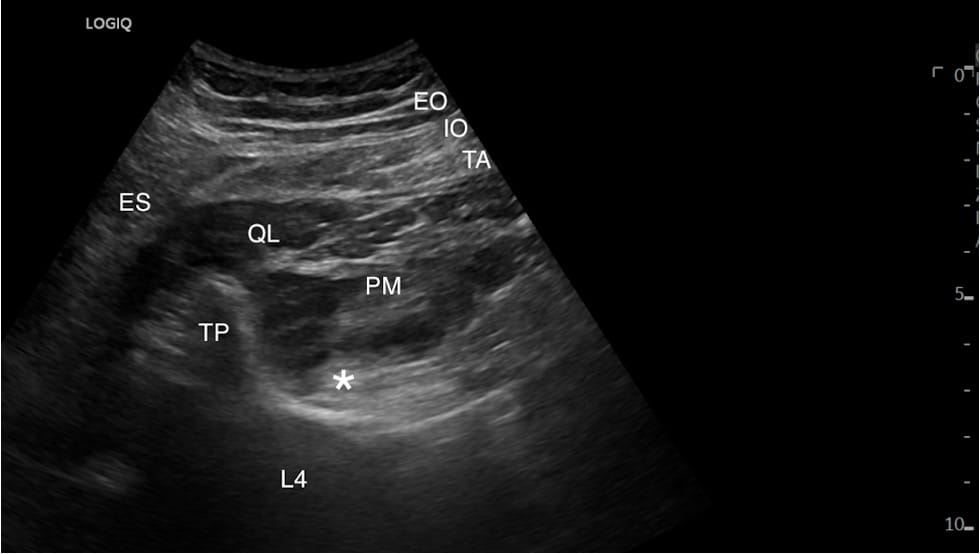
ES = erector spinae muscles, QL = quadratus lumborum muscle, PM = psoas major muscle, TP = transverse process, L4 = lumbar 4 vertebral body, * = lumbar plexus, EO = external oblique muscle, IO = internal oblique muscle, TA = transversus abdominis muscle
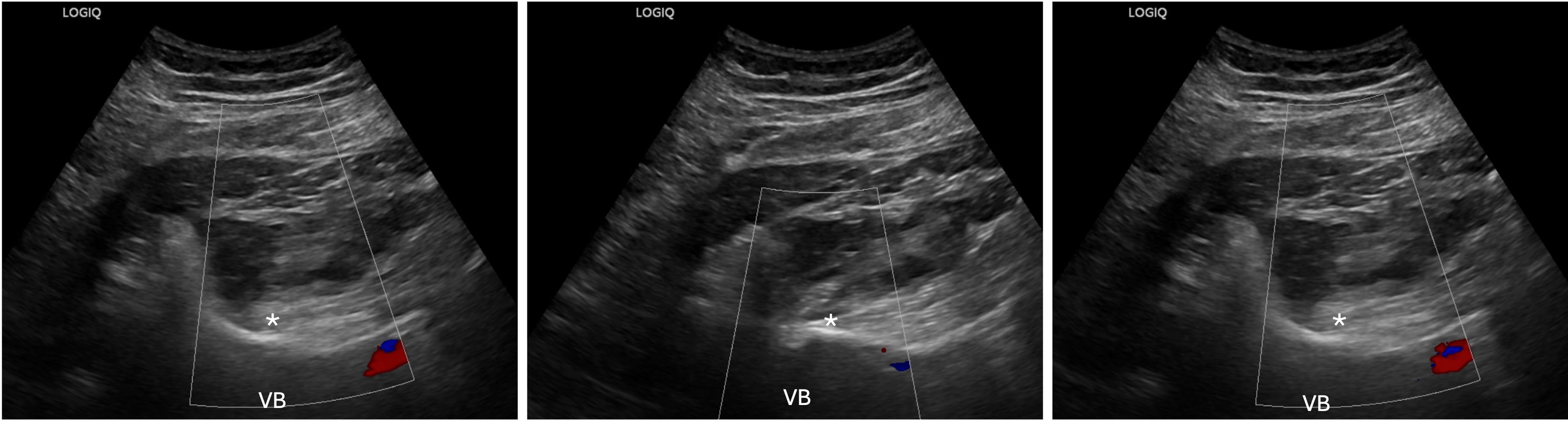
VB = vertebral body, * = lumbar plexus
After optimal sonoanatomy is obtained, a 1% lidocaine skin wheal (2-3 mL) is administered next to the posterior edge of the ultrasound probe. Under real-time ultrasound guidance, an appropriately sized needle (We use an echogenic 21G stimulating needle at least 100 mm in length for single injection blocks and a 17 Ga Tuohy needle and a 19 Ga catheter for continuous regional anesthetic blocks.) connected to a peripheral nerve stimulator is inserted at the posterior edge using an in-plane approach. We use a posterior transversal approach, where the needle is inserted along the transverse process in order to avoid lumbar arteries and veins, as most often the lumbar arteries and veins are inter-transversal.2 The needle is advanced using nerve stimulation (see “nerve stimulation” below) until the tip is seen lateral to the lumbar plexus nerves (Figure 4 and Video).
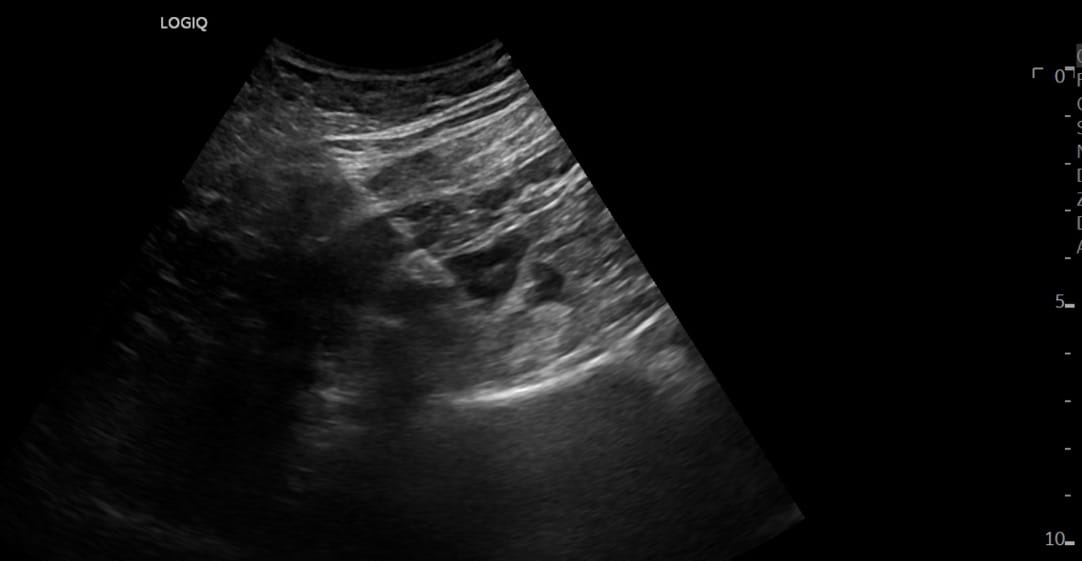
Proper placement of the needle tip is confirmed by contraction of the quadriceps muscle (see nerve stimulation below). 20-25 mL of 0.5% ropivacaine is injected slowly in 5 mL aliquots with intermittent aspiration while maintaining injection pressure <20 psi using a compressed air injection technique (see “injection pressure monitoring” below) to reduce the risk of inadvertent intraneural and unwanted epidural spread.20,21
Triple Monitoring
One of the most significant advancements in lumbar plexus block safety is triple monitoring, which includes ultrasound, nerve stimulation, and injection pressure monitoring.2
Ultrasound Guidance
Ultrasound is used for precise anatomical visualization with color doppler aiding in vascular avoidance to improve the safety and efficacy of this block.
Nerve Stimulation
Nerve stimulation confirms proper needle-nerve proximity while minimizing the risk of intraneural injection. We recommend initial stimulation at 1.5mA to elicit a motor response from the quadriceps. In coordination with needle advancement, the current is reduced gradually to 0.5-1.0 mA while maintaining quadriceps motor response to ensure adequate proximity to the lumbar plexus. Subtle changes can be assessed by placing a hand over the distal anterior thigh, assessing for quadriceps stimulation. If a patient has a history of neuropathy, higher currents may be required.
Injection Pressure Monitoring
Monitoring injection pressure ensures reduced risk of unwanted epidural spread,21 and limiting the pressure may help minimize the risk of nerve injury. Thus, it is important to maintain injection pressure of less than 20 psi. Devices are available to monitor pressure control; however, a simple alternative includes compressed air injection technique by adding air to the syringe filled with local anesthetic, and during injection, avoid compressing the air volume in the syringe to less than ½ its original volume, thus guaranteeing the injection pressure is less than 15 psi.14 This principle applies to all sizes of syringes, but taking care to position the syringe facing slightly downward to prevent injection of the air is important.
By incorporating all three modalities, anesthesiologists can significantly reduce neurovascular complications, optimize block success, and enhance patient safety beyond conventional methods.
Safety Considerations and Clinical Pearls
- The block should be performed at L4 or L5 to reduce the risk of kidney injury.14
- Real-time ultrasound guidance during advancement of the needle with concurrent nerve stimulation to elicit quadriceps motor response assists in avoiding nerve injury and ensuring needle tip placement, especially in patients with larger BMIs where needle visualization may be difficult.
- The lumbar arteries arise from the aorta and must be identified using color Doppler to avoid vascular complications.
- Maintaining injection pressure <20 psi can reduce the risk of local anesthetic spread to the epidural space as well as minimize the risk of nerve injury.21
Conclusions
The lumbar plexus block, when performed with triple monitoring to minimize the risks of neurologic and vasculature complications, provides safe and effective lower extremity analgesia.



References
- Chayen D, Nathan H, Chayen M. The psoas compartment block. Anesthesiology 1976;45(1):95-9. https://doi.org/10.1097/00000542-197607000-00019
- Nielsen MV, Bendtsen TF, Børglum J. Superiority of ultrasound-guided Shamrock lumbar plexus block. Minerva Anestesiol 2018;84(1):115-21. https://doi.org/10.23736/S0375-9393.17.11783-9
- Awad IT, Duggan EM. Posterior lumbar plexus block: anatomy, approaches, and techniques. Reg Anesth Pain Med 2005;30(2):143-9. https://doi.org/10.1016/j.rapm.2004.11.006
- Winnie AP, Ramamurthy S, Durrani Z. The inguinal paravascular technic of lumbar plexus anesthesia: the "3-in-1 block." Anesth Analg 1973;52(6):989-96.
- Kaki AM, Lewis GW. Inguinal paravascular (lumbar plexus) neurolytic block--description of a catheter technique: case report. Reg Anesth Pain Med 1998;23(2):214-8. https://doi.org/10.1097/00115550-199823020-00018
- Ritter JW. Femoral nerve "sheath" for inguinal paravascular lumbar plexus block is not found in human cadavers. J Clin Anesth 1995;7(6):470-3. https://doi.org/10.1016/0952-8180(95)00055-m
- Tokat O, Türker YG, Uckunkaya N, et al. A clinical comparison of psoas compartment and inguinal paravascular blocks combined with sciatic nerve block. J Int Med Res 2002;30(2):161-7. https://doi.org/10.1177/147323000203000208
- Hanna MH, Peat SJ, D'Costa F. Lumbar plexus block: an anatomical study. Anaesthesia 1993;48(8):675-8. https://doi.org/10.1111/j.1365-2044.1993.tb07178.x
- Kirchmair L, Entner T, Wissel J, Moriggl B, et al. A study of the paravertebral anatomy for ultrasound-guided posterior lumbar plexus block. Anesth Analg 2001;93(2):477-81. https://doi.org/10.1097/00000539-200108000-00047
- Capdevila X, Macaire P, Dadure C, et al. Continuous psoas compartment block for postoperative analgesia after total hip arthroplasty: new landmarks, technical guidelines, and clinical evaluation. Anesth Analg2002;94(6):1606-13. https://doi.org/10.1097/00000539-200206000-00045
- Sauter, AR. “Shamrock Method” - a new and promising technique for ultrasound-guided lumbar plexus blocks. Br J Anaesth, 2013; (111) eLetters supplement.
- Karmakar MK, Li JW, Kwok WH, et al. Ultrasound-guided lumbar plexus block using a transverse scan through the lumbar intertransverse space: a prospective case series. Reg Anesth Pain Med 2015;40(1):75-81. https://doi.org/10.1097/AAP.0000000000000168
- Karmakar MK, Ho AM, Li X, et al. Ultrasound-guided lumbar plexus block through the acoustic window of the lumbar ultrasound trident. Br J Anaesth 2008;100(4):533-7. https://doi.org/10.1093/bja/aen026
- Aida S, Takahashi H, Shimoji K. Renal subcapsular hematoma after lumbar plexus block. Anesthesiology1996;84(2):452-5. https://doi.org/10.1097/00000542-199602000-00027
- Awad IT, Duggan EM. Posterior lumbar plexus block: anatomy, approaches, and techniques. Reg Anesth Pain Med 2005;30(2):143-9. https://doi.org/10.1016/j.rapm.2004.11.006
- Williams PL. Gray’s Anatomy: The Anatomical Basis of Medicine and Surgery, 38th ed. London: Churchill Livingstone; 1995.
- Alkadhim M, Zoccali C, Abbasifard S, et al. The surgical vascular anatomy of the minimally invasive lateral lumbar interbody approach: a cadaveric and radiographic analysis. Eur Spine J 2015;24 Suppl 7:906-11. https://doi.org/10.1007/s00586-015-4267-5
- Baniel J, Foster RS, Donohue JP. Surgical anatomy of the lumbar vessels: implications for retroperitoneal surgery. J Urol 1995;153(5):1422-5.
- Diwan S, Nair A, Dadke M, et al. Intricacies of ultrasound-guided lumbar plexus block in octogenarians: a retrospective case series. J Med Ultrasound 2021;30(1):26-29. https://doi.org/10.4103/JMU.JMU_174_20
- Tsui BC, Knezevich MP, Pillay JJ. Reduced injection pressures using a compressed air injection technique (CAIT): an in vitro study. Reg Anesth Pain Med 2008;33(2):168-73. https://doi.org/10.1016/j.rapm.2007.10.006
- Gadsden JC, Lindenmuth DM, Hadzic A, et al. Lumbar plexus block using high-pressure injection leads to contralateral and epidural spread. Anesthesiology 2008;109(4):683-8. https://doi.org/10.1097/ALN.0b013e31818631a7