How I Do It: X-Ray-Guided Thoracic Nerve Root Block
Cite as: Nakamura H, Hashizume K, Uekita I. How I do it: x-ray-guided thoracic nerve root block. ASRA Pain Medicine News 2025;50. https://doi.org/10.52211/asra050125.008.
How I Do It
Introduction
Thoracic nerve root blocks are performed to relieve pain caused by conditions such as herpes zoster, intercostal neuralgia, post-thoracotomy or post-traumatic pain in the intercostal nerve region, and pain due to thoracic or rib metastasis.1
In the following sections, we will discuss the technique of thoracic nerve root blocks under fluoroscopic guidance.
Anatomy
The thoracic vertebrae have 12 pairs of thoracic nerve roots that exit through the intervertebral foramen and divide into anterior and posterior branches.2 The anterior branches become intercostal nerves, while the posterior branches distribute to the facet joints via the medial branch and to the paraspinal skin and erector spinae muscles via the lateral branch.3 From a dorsal view, the thoracic nerve roots are covered by the transverse and inferior articular processes as they exit into the intercostal space (Figure 1).4 The intercostal arteries branch from the descending aorta and run along the thoracic wall with the intercostal nerves. Many segmental spinal branches from the intercostal arteries enter the spinal canal through the left intervertebral foramina with some becoming radicular arteries that reach the spinal cord.5,6 The largest radicular artery, the artery of Adamkiewicz, is often found in the lower thoracic region.7 Caution should be exercised during blocks to avoid puncturing these arteries as it may lead to hemorrhage or embolism.
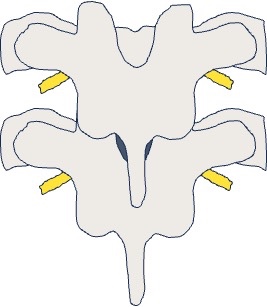
How to Match Body Position and Fluoroscopy
A pillow is placed under the patient’s upper abdomen, and the patient is positioned prone, creating a natural arch with the mid-thoracic vertebra as the apex (Figure 2).

The right-left angle is adjusted so that the spinous process is visible bilaterally in the center of the pedicles under the posterior fluoroscopic view.
As described in the anatomy section, in the posterior view, the nerve root emerging from the intervertebral foramen into the intercostal space appears to be covered by the transverse process. The cranial-caudal angle is adjusted such that the inferior margin of the transverse process and the edge of the inferior articular process are visible in the intercostal space. The nerve root is located on the ventral-caudal side.
In the upper thoracic vertebrae, when adjusting the fluoroscope cranially and caudally in the mid-thoracic vertebrae, the nerve root is often visible (Figures 3a and 3b). In the lower thoracic vertebrae, the anterior curvature of the thoracolumbar junction usually allows for visibility of the inferior margin of the transverse process. In cases of kyphosis or scoliosis, further axis adjustments are required.
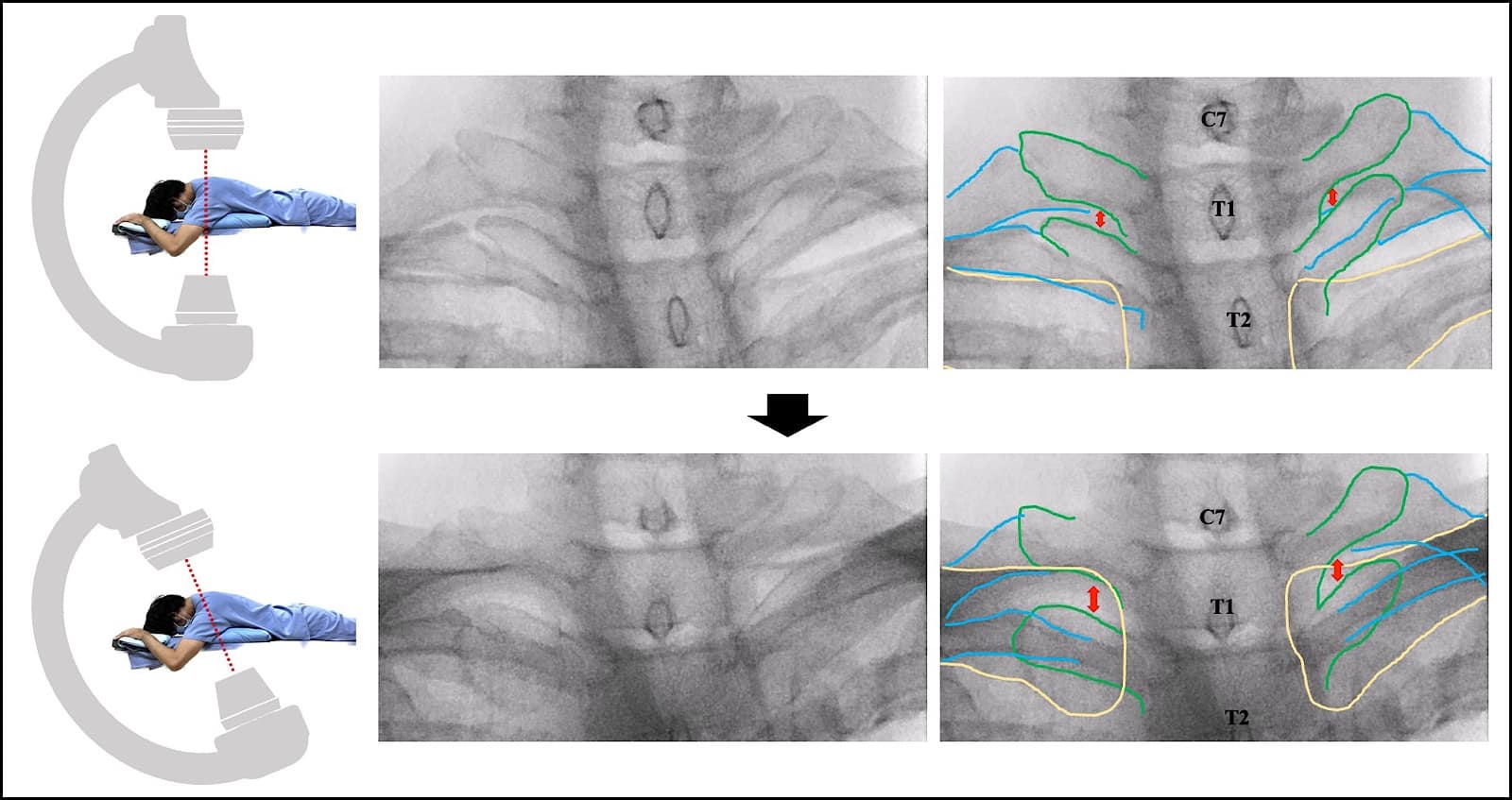
Green line = transverse process; blue line = rib; yellow line = clavicle
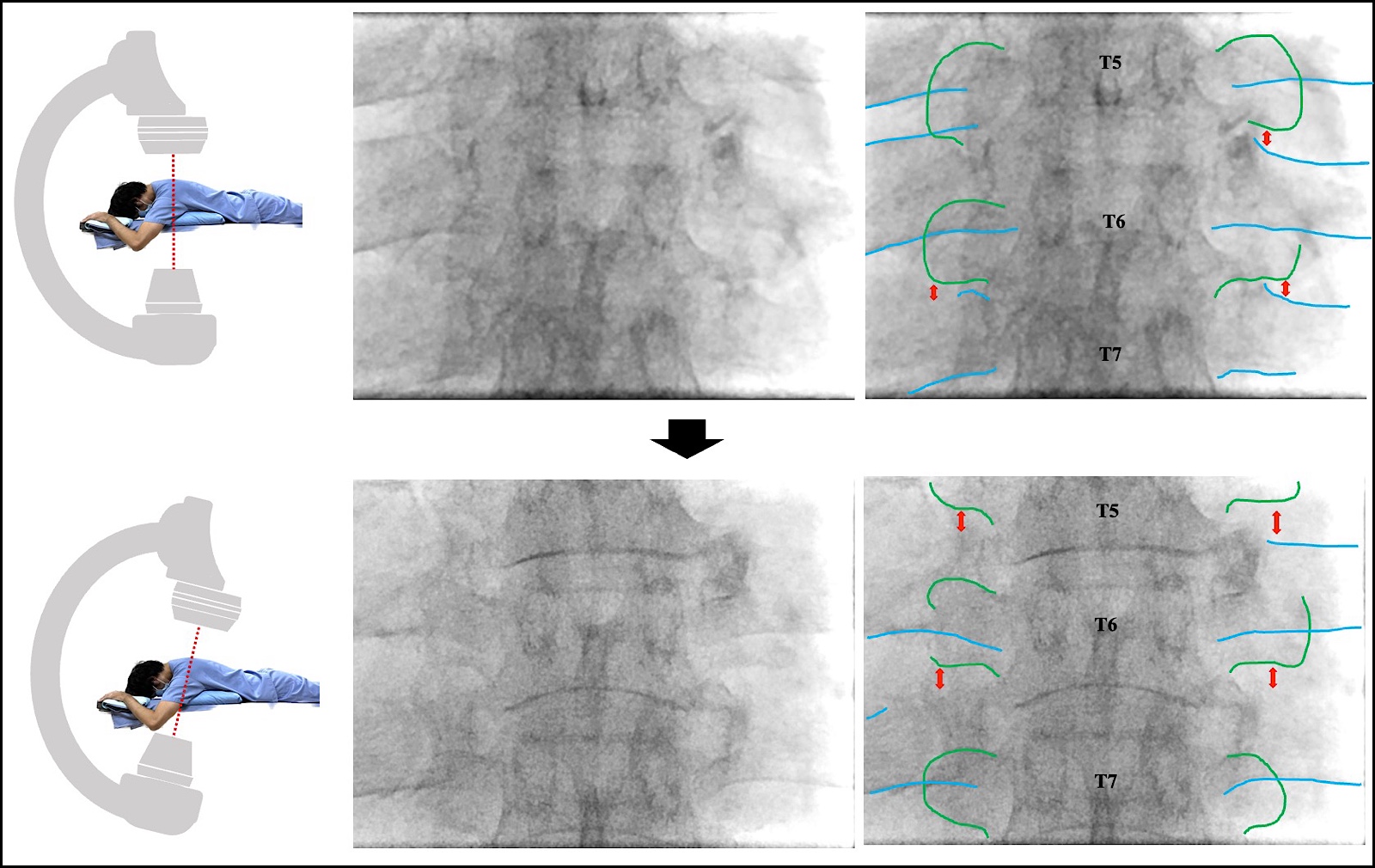
Green line = transverse process; blue line = rib; yellow line = clavicle
Procedure
Equipment and Drugs
- Needles: 25G 60 mm or 23G, 22G 60 mm–100 mm
- Local anesthetic: 1% mepivacaine
- Contrast agent: iohexol 240 mgI/mL
- Block agents: 0.5% mepivacaine and dexamethasone 1.65 mg, 1 mL (dexamethasone is available as 3.3 mg/ml in my hospital).
- The following disinfectants are required: 0.5% chlorhexidine + ethanol or povidone-iodine solution, cotton balls, gauze, Kocher forceps, and drape.
Procedure Details
The needle is inserted at the lower margin of the transverse process. Under local anesthesia, the needle is advanced above the transverse process under fluoroscopy, making contact with the base of the transverse process. The needle is then moved caudally, bypassing the inferior border of the transverse and inferior articular processes and advancing toward the intervertebral foramen (Figure 4, Video 1).
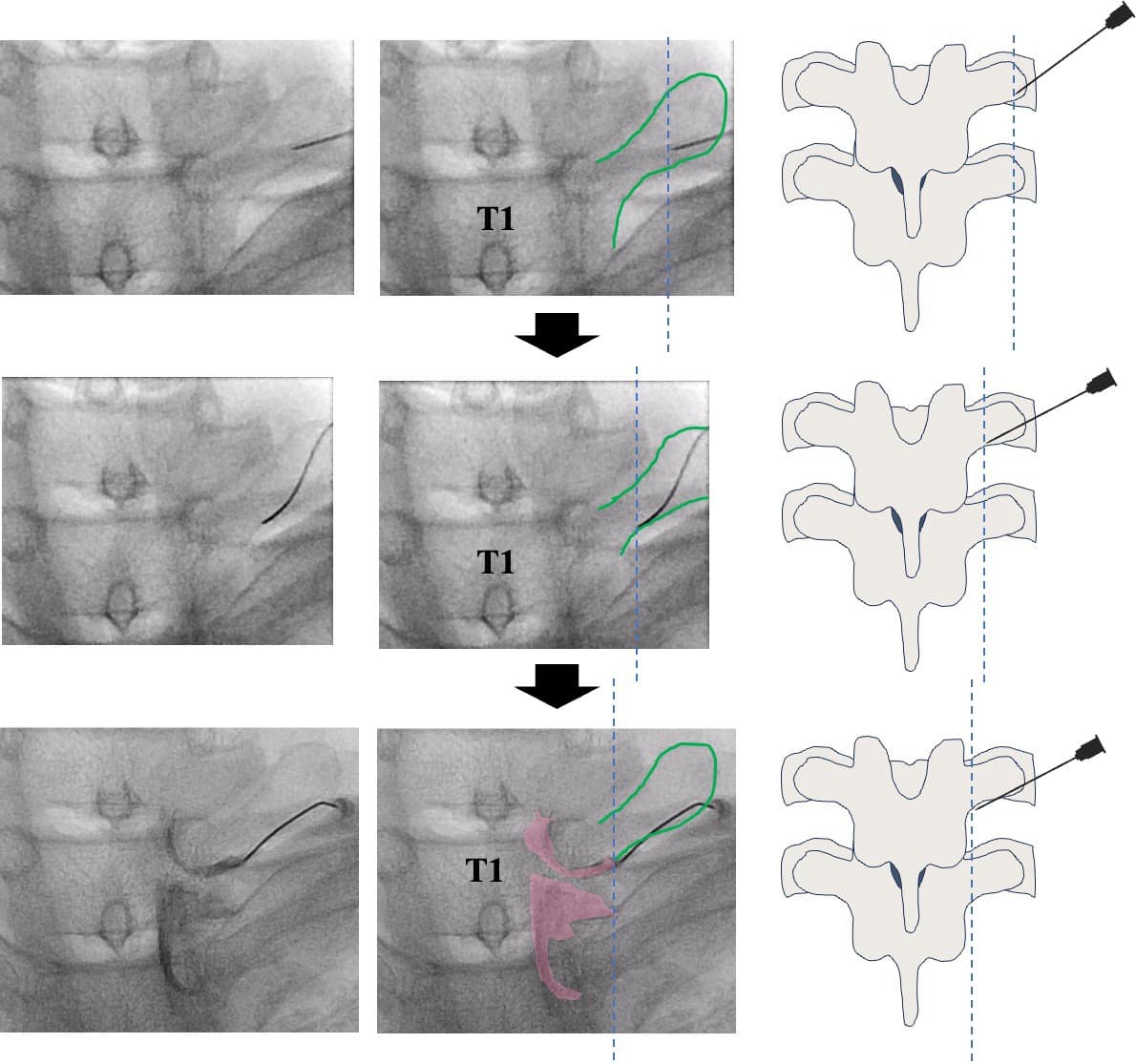
Green line = transverse process; pink area = contrasted epidural space; dotted line = advancing position of the needle
TP = transverse process, Rib = ribs, ST = sternum
Points to Note and Clinical Pearls
- In smaller patients, the tip of the transverse process may be encountered at shallow depths. If the tip is misidentified as the base of the transverse process, advancing the needle may cause pneumothorax.
- Caution must be exercised regarding the radicular artery, which is often located in the upper part of the intervertebral foramen.
- Deep penetration into the intervertebral foramen (medial to the pedicle on frontal fluoroscopy) can risk dural puncture or injury to the spinal cord
- The needle may pass through the nerve root and reach the vertebral body using only frontal images. In addition to frontal fluoroscopy, lateral fluoroscopy is recommended to verify the needle depth and avoid pneumothorax or mediastinal puncture (Figure 5).
Interpretation of Contrast and Injection of Drugs
The contrast is injected under real-time fluoroscopy once the needle reaches the intervertebral foramen. The tip of the needle should be lateral to the pedicle. Contrast images often show a perineural pattern of the thoracic nerve root block (Figure 5). If the image is appropriate, 0.5–1 mL of 0.5% mepivacaine and 1.65 mg of dexamethasone should be injected. Pulsed or thermal radiofrequency treatments may be applied if necessary. After the nerve block, vital signs should be monitored, and bed rest should be ensured for 45 minutes.
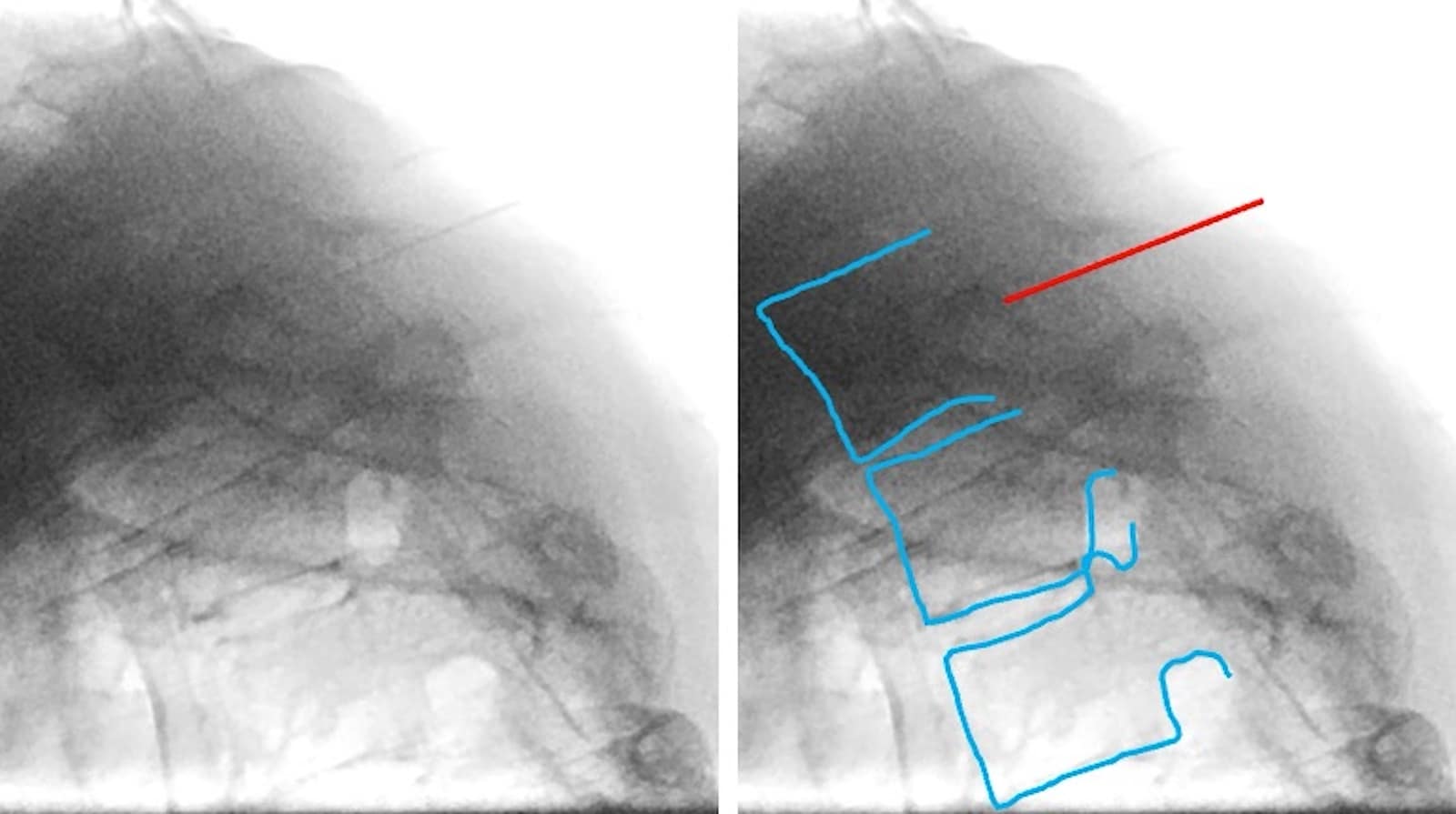
Red line = needle; blue line = vertebrae.
Points to Note and Clinical Pearls:
- The subdural or subarachnoid contrast spread should be carefully assessed if the needle tip is near the pedicle.
- If the needle tip is directed laterally, the risk of pneumothorax increases, potentially presenting as a dome-shaped pleural contrast. A cough during drug injection suggests pneumothorax, warranting further observation.
- Arterial injection of contrast results in transient imaging near the intervertebral foramen, disappearing quickly. This should not be overlooked.
- Venous contrast spread, characterized by irregular diffusion and slow disappearance, may indicate contact with the external vertebral venous plexus. Advancing the needle, 2–3 mm often reaches the nerve root (Figure 6).
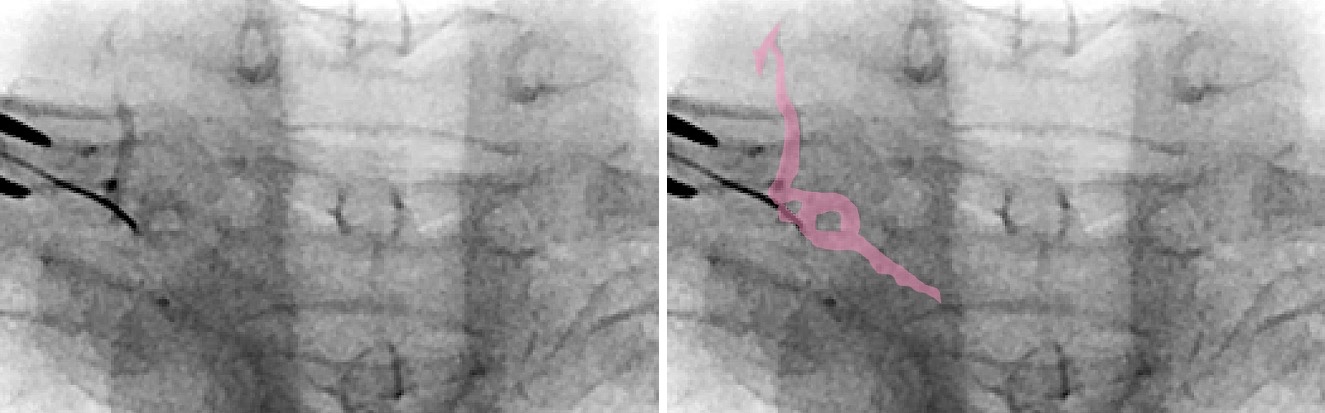
Pink area = contrasted veins
Complications
Potential complications include subcutaneous hemorrhage, subcutaneous abscess, hypotension, malaise, bradycardia, pneumothorax, subarachnoid injection, post-dural puncture headache, spinal cord injury, spinal ischemia due to inadvertent intra-arterial injection or arterial spasm, epidural hematoma due to vascular injury, epidural abscess, and myelitis.
Discussion
Our x-ray-guided thoracic nerve root block allows for constant visualization of the needle. It is performed by initially positioning the needle on the transverse process and then sliding it along the bone. Using contrast agents, anatomical structures can be clearly visualized, ensuring accurate nerve block targeting and facilitating the early detection of complications. This technique frequently visualizes the epidural space and thus could be termed a “thoracic transforaminal epidural block.” Recent reports suggest that nerve root blocks are more effective than paravertebral blocks in pulsed radiofrequency therapy for chronic post-mastectomy pain.8 Additionally, Horner’s sign is sometimes observed with T1 nerve root blocks, making them a possible alternative to the stellate ganglion block.9,10
Conclusion
X-ray-guided thoracic nerve root block is a valuable and precise technique for managing neuropathic pain in the thoracic region. This method enhances targeting accuracy and early complication detection by enabling continuous needle visualization and anatomical confirmation with contrast agents, thereby offering an effective therapeutic option for pain management.



References
- Ifuku M, Iseki M. Thoracic nerve root block (x-ray guided). In: Ohseto K, Uchino H, Iida H, eds. Nerve Blockade and Interventional Therapy. Berlin, Germany: Springer; 2019.
- Joshua AW, Vamsi R, Bennett F. Anatomy, Back, Thoracic Vertebrae. Treasure Island, FL: StatPearls Publishing; 2023.
- Niklas L G, Sajedur R, Peter P L. Anatomy, Thorax, Intercostal Nerves. Treasure Island, FL: StatPearls Publishing; 2023.
- Mazda KT, Mena GK, Brian TD, et al. Thoracic spinal endoscopy-anatomical considerations. In: Jin-Sung K, Jun H L, Yong A, eds. Endoscopic Procedures on the Spine. Berlin, Germany: Springer; 2020.
- Mohr JP, Benavente O, Barnett HJ. Spinal cord ischemia. In: Barnett HJ, Mohr JP, Stein BM, et al., eds. Stroke Pathophysiology, Diagnosis, and Management. Philadelphia, PA: Churchill Livingstone; 1998.
- Parent A. Blood supply of the central nervous system. In: Stroke Pathophysiology, Diagnosis, and Management, Carpenter's Human Neuroanatomy. 9th ed. Philadelphia, Pennsylvania, United States: Williams and Wilkins; 1996.
- Hurst RW. Spinal vascular disorders. In: Atlas SW, ed. Resonance Imaging of the Brain and Spine. Philadelphia, PA: Lippincott; 2006.
- Hetta DF, Mohamed SAB, Mohamed KH, et al. Pulsed radiofrequency on thoracic dorsal root ganglion versus thoracic paravertebral nerve for chronic postmastectomy pain, a randomized trial: 6-month results. Pain Physician 2020;23:23-35.
- Hashizume K, Fujiwara A, Watanabe K, et al. A prospective comparison of CT-epidurogram between Th1-transforaminal epidural injection and Th1/2-parasagittal interlaminar epidural injection for cervical upper limb pain. Pain Physician 2019;22:165-76.
- Kim ED, Yoo WJ, Kim YN, et al. Ultrasound-guided pulsed radiofrequency treatment of the cervical sympathetic chain for complex regional pain syndrome: a retrospective observational study. Medicine (Baltimore) 2017;96:e5856. https://doi.org/10.1097/MD.0000000000005856