The Value of Regional Anesthesia Fellowship: Is it a Question of Redefining, Rebranding or Rebuilding?
Cite as: Nanda M, Le Wendling L. The value of regional anesthesia fellowship: is it a question of redefining, rebranding, or rebuilding?. ASRA Pain Medicine News 2026;51. https://doi.org/10.52211/asra050126.008.
Introduction
With attractive practice opportunities available directly after residency and a plethora of readily available online learning resources, many graduates are re-evaluating the need for subspecialty fellowship training. Regional anesthesia programs, once considered a natural next step for procedural-minded residents, are experiencing a stagnancy in applications and increased scrutiny from prospective fellows.
When Ready1 first proposed the concept of a formal, anesthesiology-based acute pain service in 1988, fellowships in regional anesthesia and acute pain medicine (RAAPM) began to emerge, with a surge in interest following the introduction of ultrasound-guided regional anesthesia from 2006 to 2010. The push for American Council for Graduate Medical Education (ACGME) accreditation began soon after, and in 2016, ACGME applications opened for RAAPM. In 2023,2 the San Francisco (SF) match was introduced to provide a more seamless and fair environment for fellow applicants. By 2025, 93 RAAPM fellowships will offer over 200 positions in the United States and Canada, of which 46 will be ACGME-accredited. More than 170 of those positions were available on the SF match. Eighty-six applicants applied through the match; this number remained steady during the first 2 years of match initiation, though the number of positions exceeded the number of participants by twofold.
This evolving landscape compels a critical reassessment of how we define the value of fellowship, and programs must articulate and deliver the benefits of a dedicated year in post-residency training.
How Do Programs Deliver on the Promise: Innovating and Investing in the Fellowship Year
Regional anesthesia fellowship programs combine niche clinical experiences with mentorship, academic exploration, leadership development, and career guidance, providing an invaluable skill set that stays with graduates for life.
Curriculum Evolution and Personalization: One Year, Many Dimensions
The era of measuring fellowship success by block counts alone has passed. What we teach and how we teach it matters. Contemporary regional anesthesia training must reflect the full complexity of perioperative pain management. This includes acute pain consultations, care transitions, and multimodal analgesia strategies, paired with a deliberate expansion of the fellow’s regional anesthesia repertoire. Advanced nerve blocks3 and skills such as point-of-care ultrasound, emerging technologies, health care economics, and interdisciplinary collaboration are now integral to a comprehensive curriculum.
Equally important is how programs adapt the fellowship experience to fit individual goals. No two fellows are alike, and the most effective training environments embrace that diversity through structured flexibility. Elective time in the latter part of the year allows fellows to pursue focused interests, whether in pediatric regional anesthesia, simulation-based education, research, or quality improvement. For those still shaping their career direction, electives offer the opportunity to explore different paths in depth. The result is a training experience that is not only clinically robust but personally meaningful, a foundation tailored for long-term growth and leadership in regional anesthesia.
Career Development and Mentorship: Building Trajectory and Community
Successful fellowships go beyond skill refinement to provide professional clarity, enduring mentorship, and strategic guidance. Fellows benefit from structured career support from CV building and contract review to discussions on practice models and developing longitudinal relationships with invested faculty. These mentors help fellows gain confidence, grow their networks, and navigate the unwritten aspects of the specialty. Graduates emerge not only as competent clinicians but as connected contributors to a vibrant, collaborative community. Early mentorship often translates into greater academic productivity and long-term career success for fellows.4
Leadership Training
Many fellowship graduates go on to lead acute pain services, implement ERAS pathways, or serve as the go-to person for complex perioperative analgesia. Leadership development should therefore be part of the training experience. Programs are increasingly embedding opportunities to participate in quality improvement projects, service design, faculty development, and interdepartmental initiatives. Fellows benefit from seeing how the system works and how to influence it before they are asked to lead on day one of their attending jobs.
Collaboration Across Institutions: Expanding Access and Community
Not every program has access to the same resources, but collectively, the community does. This collaborative spirit was on full display at the Regional Anesthesia Fellowship Firestarter Course, hosted at the University of North Carolina in August 2025 (Figure 1). Twenty fellows from across the United States and Canada participated in cadaver-based dissection, needling, and ultrasound scanning, refining their skills and connecting with peers. Beyond in-person workshops, multi-institutional virtual journal clubs, shared didactic libraries, and traveling elective opportunities are additional ways programs can extend learning beyond institutional boundaries. These initiatives foster camaraderie, broaden exposure, and deepen the fellowship experience through shared resources and purpose.

Financial Incentives: Bridging the Gap to Make Fellowship Feasible
ACGME-accredited programs typically offer a salary commensurate with a PGY-5 position, plus additional moonlighting opportunities, with a median of $91K to $ 93K and a range of $77K to $125K. Non-ACGME fellowship programs provide higher salaries and more faculty time during the year, with a median salary of $115K to $120K and a range of $38K to $250K.5 Compared to the salary for a recent graduate in the academic setting (median $457K for assistant professor rank for year 2022-23)6 and private practice setting (average $523K for year 2025),7 without increased initial salary for fellowship-trained graduates, the benefit of fellowship resides in its ability to provide the fellow with a greater clinical set of skills for improved safety and clinical outcomes and a pathway for academic advancement.
With today’s high-paying job market, the decision to pursue a fellowship often hinges on financial feasibility. As American Society of Anesthesiologists president Dr. Patrick Giam noted,8 bridging the salary gap through institutional sponsorship models, where hospitals or practices help subsidize fellowship training in return for post-fellowship employment commitments, may be key to reversing declining application trends. But while not every program has the means to offer full stipends, many are already leveraging creative, attainable solutions. Hybrid clinical instructorships, internal moonlighting shifts, or incentivized call coverage allow fellows to earn supplemental income without compromising their education. These mechanisms not only help offset opportunity costs but also demonstrate that programs understand and respect the financial realities their trainees face.
The Value of a Dedicated Fellowship: Skills, Identity, and Lasting Impact
In today’s training environment, where ultrasound-guided techniques are routinely taught during residency and online educational content is abundant, the value of a dedicated regional anesthesia fellowship can be questioned. While it may seem feasible to build proficiency through self-directed learning, on-the-job experience, or digital resources, fellowship offers something fundamentally different: immersion.
In a structured, goal-oriented environment surrounded by expert mentors, fellows move beyond procedural competence to develop refined clinical judgment, confidence in complex decision-making, and a shared professional identity within the subspecialty. There is a profound difference between performing a block under supervision during a busy clinical day and spending dedicated time understanding why this approach works for this patient, when an alternative might be superior, and how to troubleshoot when expected landmarks aren't visible. Fellowship provides the space to ask these questions, observe expert decision-making in real time, and develop the pattern recognition that separates technical proficiency from clinical mastery.
Consider the patient with chronic opioid use, poorly controlled anxiety, and obstructive sleep apnea presenting for major shoulder surgery. The technically proficient clinician can place a block; the master clinician anticipates rebound pain, respiratory vulnerability, catheter management challenges, and the psychosocial context that may amplify postoperative distress. Fellowship training provides repeated exposure to these layered scenarios, teaching fellows how to construct multimodal plans that balance analgesia, safety, and patient expectations rather than relying on a single procedural solution. This integration of physiology, pharmacology, and communication is what transforms a block into comprehensive acute pain management.
The Difference Between Doing and Understanding
The fellowship year fosters growth that cannot be replicated through asynchronous or incidental learning. Fellows gain exposure to faculty thought processes during complex consultations. They hear how experienced clinicians weigh competing risks, communicate uncertainty, and balance evidence with patient preferences. They navigate real-time complications, learning not just what went wrong but why and how to prevent it. They participate in team-based care, understanding how regional techniques fit into enhanced recovery pathways and how to build trust with skeptical surgeons and nursing staff managing patients postoperatively.
Beyond Technical Skills: Becoming a Consultant
Perhaps most importantly, fellowship cultivates the confidence to function as a true consultant in acute pain medicine, the person others turn to when standard approaches fail. This confidence comes from managing edge cases with expert guidance: the brachial plexus injury where standard approaches won't work, the chronic pain patient who needs a complex catheter strategy, and the anticoagulated patient who requires precise timing and shared decision-making. These scenarios demand more than technical skill: They require judgment, communication, and the ability to navigate ambiguity.
Fellows also develop a professional identity and network that extends beyond their training institution. They attend conferences as active participants, present research, meet thought leaders, join societies, and begin to see themselves as contributors to the specialty rather than just practitioners. This identity shift is subtle but powerful: Fellowship graduates don't just perform regional anesthesia; they advance it through quality improvement, education, and leadership.
The Compound Effect Over a Career
When thoughtfully designed, fellowship is transformative, developing both skillset and mindset. The investment pays dividends throughout a career: greater versatility, reduced anxiety with complex cases, faster recognition as the expert, and leadership opportunities that might otherwise take years to access. Fellowship graduates enter their first attending roles not as novices learning on the job, but as consultants ready to contribute, and often lead, from day one.
Fellowship also establishes the habits that sustain lifelong growth. By engaging in research discussions, journal clubs, quality initiatives, and interdisciplinary dialogue, fellows internalize the expectation that practice must evolve in response to evidence. This mindset often distinguishes those who simply keep up from those who help advance the specialty.
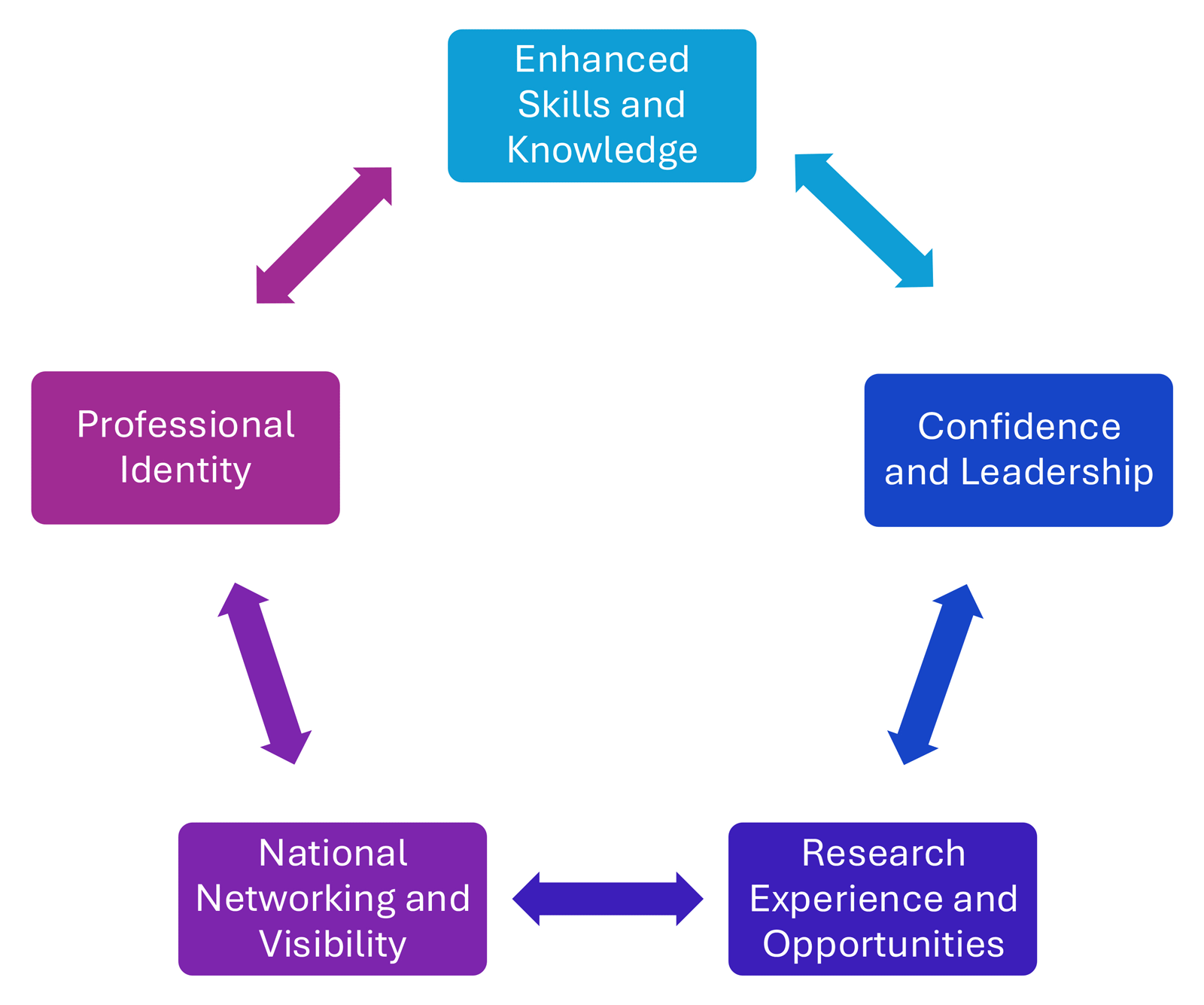
The year equips graduates not only with technical fluency but also with clarity of perspective, professional confidence, and leadership capabilities that enhance their careers in the ever-changing landscape of anesthesiology practice (Figure 2). In an era when the financial opportunity cost is undeniable, the question becomes: What is the cost of not having that foundation when you're the only one in the room being asked to solve a problem no one else can?
For some, the answer will be that they can build these skills through practice over time. For others, the realization that fellowship compresses years of trial-and-error learning into one structured, supported year, while building a professional network and identity that lasts a lifetime, makes the investment not just worthwhile, but essential.


References
- Ready LB, Oden R, Chadwick HS, et al. Development of an anesthesiology-based postoperative pain management service. Anesthesiology 1988;68:100-6. https://doi.org/10.1097/00000542-198801000-00016
- Budde B, Elkassabany N, Hargett M. Match process implemented by majority of United States RAAPM fellowship programs for 2023-2024 academic year recruitment. ASRA Pain Medicine News 2022;47. https://doi.org/10.52211/asra020123.013
- Turbitt LR, Mariano ER, El-Boghdadly K. Future directions in regional anaesthesia: not just for the cognoscenti. Anaesthesia 2020;75:293-7. https://doi.org/10.1111/anae.14768
- Mentorship in regional anesthesia and pain medicine: a perspective from trainees and their trainers. ASRA Pain Medicine News. https://asra.com/news-publications/asra-newsletter/newsletter-item/asra-news/2019/01/31/mentorship-in-regional-anesthesia-and-pain-medicine-a-perspective-from-trainees-and-their-trainers. Published January 31, 2019. Accessed December 24, 2025.
- Informal survey of the Regional Anesthesia Fellowship Directors Association conducted December 2025-January 2026.
- Owda D, Mensah MO, Yang D, et al. Salary differences by gender, race, and ethnicity among assistant professors at US medical schools. JAMA Netw Open 2025;8(5):e259583.https://doi.org/10.1001/jamanetworkopen.2025.9583
- Doximity 2025 Physician Compensation Report. https://www.doximity.com/reports/physician-compensation-report/2025. Published July 31, 2025. Accessed February 22, 2026.
- Giam, P. Investing in the future of anesthesiology: why fellowships matter. Anesthesiology News.https://www.anesthesiologynews.com/Commentary/Article/11-25/Investing-in-the-Future-Of-Anesthesiology-Why-Fellowships-Matter/78776. Published November 12, 2025. Accessed December 24, 2025.